In the world of literature and language, we rely heavily on similes and metaphors to make sense of complex human experiences. We say love is a battlefield, or time is a thief. But when evaluating human biology, the most accurate comparison is that emergency medical readiness is like a safety net. It remains entirely unnoticeable until the exact terrifying moment the tightrope snaps. If you want to protect your loved ones, securing accredited London CPR training is the ultimate way to build that net. Let’s explore why residents in this academic city are upgrading their life-saving skills and learning to rewrite the endings of modern tragedies.
London, Ontario, is a city deeply defined by its academic and cultural institutions. With the massive, sprawling presence of Western University and Fanshawe College, it is a community that places an incredibly high premium on learning, literacy, and the humanities. We spend years studying classic literature, analyzing poetry, and pursuing advanced degrees to prepare ourselves for the narrative arc of our professional lives. We view education as the armor that will protect us from the uncertainties of the future.
Yet, despite this profound dedication to intellectual preparation, thousands of London residents are walking around completely unprepared for the most critical, plot-altering moment they will ever face: a sudden medical emergency. When a sudden cardiac arrest, a severe choking incident, or a massive allergic reaction occurs, the theoretical knowledge we gain in lecture halls becomes instantly useless. The survival of a loved one or a stranger on the street does not depend on our ability to articulate a thesis or defend a dissertation; it depends entirely on our physical ability to act as an immediate, mechanical safety net. Today, a growing movement of writers, academics, and everyday citizens in London are recognizing this gap. They are stepping out of the theoretical realm and into the physical one to ensure they are equipped for real-world crises.
The Metaphor of the Unseen Thread
To understand the suddenness of a medical emergency, one must think of human health like an unseen thread holding up a heavy, intricate chandelier. For decades, the thread holds strong. We go to work, we walk along the Thames River, we sit in the crowded cafes on Richmond Row, and we never give the thread a single second thought. But human biology is incredibly delicate. A hidden congenital defect, a sudden severe trauma, or an unexpected physiological failure can cause that thread to snap without a single line of foreshadowing.
When sudden cardiac arrest strikes, it is not like a slow, dramatic chapter building to a climax over several pages. It is an immediate, catastrophic disruption of the narrative. The heart’s electrical system misfires, the biological pumping mechanism completely seizes, and the person collapses to the floor. In literature, such an event is often used as a tragic plot device to spur the protagonist into action. In reality, it is a chaotic, terrifying scenario where the brain begins to suffer irreversible damage after just four short minutes without oxygenated blood.
Without a safety net in place—without a trained bystander who knows exactly how to step in and artificially sustain that oxygen flow—the story ends right there. The safety net is not built from hope, good intentions, or well-wishes; it is woven entirely from the physical muscle memory of deep, rhythmic, unrelenting chest compressions.
Why Relying on the Protagonist (Paramedics) Is a Flawed Plot
We are culturally conditioned by movies and television to view paramedics and emergency medical technicians (EMTs) as the ultimate protagonists of our healthcare stories. When the unthinkable happens, we are taught to immediately dial 911 and simply wait for the heroes in the ambulance to arrive and save the day. They possess the advanced medical equipment, the clinical training, and the life-saving intravenous drugs required to reverse severe medical events.
However, relying entirely on this external protagonist is a fundamentally flawed plot structure, primarily due to the uncompromising laws of time and geography. London is a sprawling, busy municipality with dense traffic corridors. If a medical emergency occurs in a packed, stadium-style lecture hall at Western University, or during a busy Friday night at a dimly lit restaurant downtown, the ambulance must navigate gridlock, pedestrian crosswalks, complex campus maps, and locked facility doors.
Even with the absolute best emergency dispatch times in the province, it will likely take paramedics anywhere from eight to fifteen minutes to physically reach the patient’s side. If a heart has stopped, a fifteen-minute delay is a biological eternity. The paramedics are undoubtedly the heroes of the story, but they arrive in the second act. The survival of the patient relies entirely on the people who are present for the prologue. When you take a formal first aid course, you are no longer a passive reader of the tragedy. You become the active first responder, the critical bridge that keeps the patient’s brain alive until the advanced medical cavalry arrives.
The Rhythm of Survival: CPR as a Poetic Meter
Writers and musicians intimately understand the profound importance of rhythm. In poetry, the iambic pentameter dictates the heartbeat of a sonnet, providing a steady, reliable cadence that carries the reader through the emotion of the text. Remarkably, emergency medicine relies on a very similar concept of strict, rhythmic pacing.
Cardiopulmonary Resuscitation (CPR) is not a chaotic, random application of physical force. It is a highly calculated, rhythmic physical intervention. When you perform chest compressions, you are acting as an external, manual pump for a stopped heart. To be effective, those compressions must be delivered at a very specific rate: between 100 and 120 beats per minute, pressing down at least two inches into the chest to manually force blood out of the heart chambers and up into the brain.
In a comprehensive CPR class, professional instructors teach this rhythm with the exact same dedication a music teacher uses with a metronome. You learn to internalize the beat, often using the tempo of famous songs like the Bee Gees’ “Stayin’ Alive” to guide your hands. It is a frantic, physically exhausting rhythm, but it is the exact tempo required to hold off brain death. Learning this rhythm is like learning a new language—one spoken entirely through physical action, precise timing, and immense focus.
Reading the Signs: The Literacy of First Aid
Just as a skilled reader can identify themes, motifs, and hidden subtext in a novel, a trained first aider possesses a unique kind of medical literacy. They learn how to “read” a patient and interpret the subtle, physical signs of a body in deep distress.
Many severe medical emergencies disguise themselves as minor inconveniences. A person experiencing a severe heart attack might not clutch their chest in dramatic agony like an actor on a stage; they might simply complain of profound indigestion, a dull ache radiating down their jaw, and a sudden, cold sweat. A person experiencing a stroke might just seem mildly confused, or have a slightly slurred pronunciation of certain words that mimics intoxication.
A standard first aid course teaches you the specific algorithms required to read these signs accurately. You learn the FAST acronym (Face drooping, Arm weakness, Speech difficulty, Time to call 911) to instantly recognize neurological failure. You learn how to identify the high-pitched, wheezing sound of anaphylaxis before the airway completely closes. This medical literacy allows you to bypass the confusion and intervene decisively, shifting the trajectory of the emergency from panic to structured, clinical response.
Editing Out the Panic: Why Formal Certification Matters
Anyone can watch a five-minute video online about how to perform the Heimlich maneuver or how to push on a chest. But there is a massive difference between reading a textbook about swimming and actually being thrown into the deep end of the freezing ocean.
When you witness a massive physical trauma or a cardiac arrest, your sympathetic nervous system triggers a massive, uncontrollable dump of adrenaline. Your hands shake, your vision tunnels, and your fine motor skills rapidly deteriorate. If your knowledge is only theoretical, that wave of panic will completely paralyze you. This is known as the “Bystander Effect,” where an entire crowd of people will simply stand around watching a tragedy unfold, each person assuming someone else will step up to help.
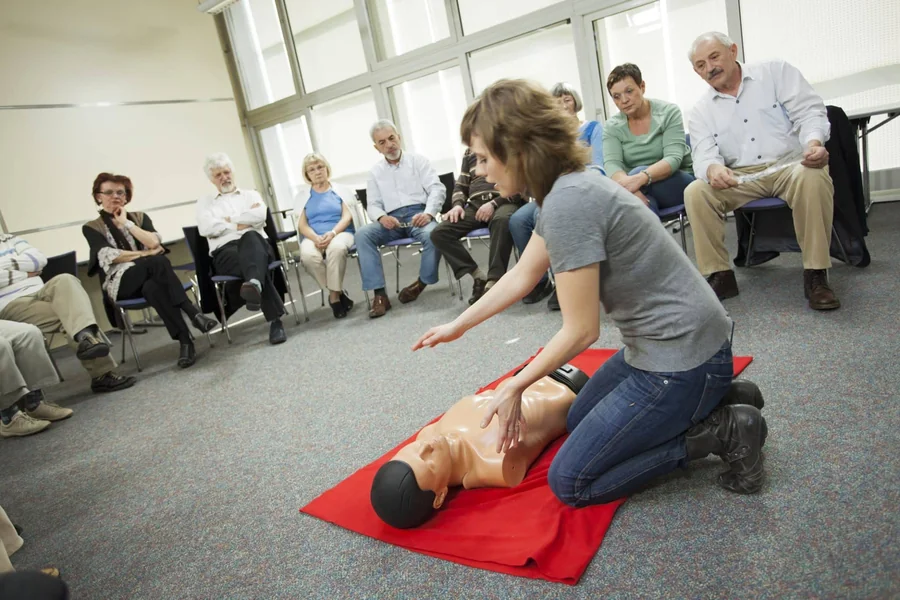
Formal certification is the editorial process that completely removes that panic from your system. By partnering with an accredited, industry-leading provider like Coast2Coast First Aid & Aquatics, you subject yourself to rigorous, physical practice. You spend hours kneeling on the floor, applying heavy pressure to specialized training mannequins. You practice ripping open the package of an Automated External Defibrillator (AED), applying the sticky pads to a bare chest, and listening to the machine’s voice prompts while a timer ticks down. This hands-on repetition builds profound muscle memory. It ensures that when the adrenaline hits you in the real world, your brain does not have to invent a solution from scratch; it simply falls back on the algorithm it has practiced a dozen times before.
Frequently Asked Questions
- Is an AED basically like a reboot button for the heart?
Yes, the simile is quite accurate. When a heart goes into sudden cardiac arrest, it is usually experiencing a chaotic, electrical misfire called ventricular fibrillation. An Automated External Defibrillator (AED) delivers a precise electrical shock that momentarily stops the heart, allowing its natural pacemaker to “reboot” and establish a normal, functional rhythm.
- Can I get sued if I perform CPR and accidentally break a patient’s rib?
It is a common fear, but the law provides a robust safety net. Ontario’s Good Samaritan Act specifically protects individuals who voluntarily provide emergency medical assistance from civil liability. As long as you act reasonably within the scope of your training and do not act with gross, malicious negligence, you are legally shielded, even if a rib fractures during deep compressions (which is quite common and preferable to brain death).
- Do modern CPR courses still teach mouth-to-mouth resuscitation?
While rescue breaths remain a critical component of the curriculum—especially for drownings and pediatric emergencies—the methodology has changed. Rescuers are now trained to use protective CPR pocket masks equipped with one-way valves. This physical barrier ensures that air goes into the patient while protecting the rescuer from bodily fluids, vomit, and communicable diseases.
- How is first aid training structured for busy university students and professionals?
To accommodate demanding academic and work schedules in London, providers utilize a “blended learning” format. Students complete the comprehensive theoretical reading and medical quizzes online at their own pace over several days. Once the digital theory is finished, they attend a highly condensed, in-person skills session to practice and demonstrate the physical interventions.
- How do I know if someone is suffering from a severe opioid overdose?
The ongoing opioid crisis requires widespread medical literacy. A severe overdose typically presents with a specific triad of signs: dangerously slow or completely absent breathing, pinpoint (constricted) pupils, and a blueish/grey tint to the lips and fingernails. Modern courses train responders to recognize this pattern and safely administer Naloxone (Narcan) nasal spray.
- What is the difference between standard CPR and Basic Life Support (BLS)?
Standard CPR is designed for the everyday layperson, focusing on single-rescuer chest compressions and simple AED use to keep a patient alive until paramedics arrive. BLS is an advanced, clinical-grade course designed for healthcare professionals. It covers complex two-rescuer dynamics, pulse checks, and the use of specialized Bag-Valve Masks (BVM) to deliver high-concentration oxygen.
- How long is a standard first aid certification valid in Ontario?
A Standard First Aid and CPR/AED certification issued by an approved provider is legally valid for exactly three years from the date of completion. To keep their life-saving skills sharp and their workplace credentials valid, individuals must complete a recertification course prior to that expiration date.
- Do first aid courses teach you how to handle a severe choking incident?
Absolutely. Choking is a terrifying, silent emergency that requires immediate physical intervention. Students learn the exact mechanics of abdominal thrusts (the Heimlich maneuver) for conscious adults, modified chest thrusts for pregnant individuals, and the delicate sequence of back blows and chest compressions required to save a choking infant.
- Can I use an AED on a wet surface, like near a swimming pool or in the snow?
Electricity and water are a dangerous combination, but AEDs are heavily shielded. If a patient is lying in a puddle or near a pool, you must swiftly drag them to a drier surface. Before applying the adhesive AED pads, you must vigorously wipe their bare chest completely dry with a towel or clothing to ensure the electrical shock penetrates the heart rather than arcing across the wet skin.
- What should a comprehensive home or dorm-room first aid kit contain?
A proactive emergency kit should move far beyond cheap, generic adhesive bandages. It needs to contain heavy trauma dressings (ABD pads) capable of stopping arterial bleeding, a CPR pocket mask, heavy-duty medical trauma shears for cutting away clothing, sterile water-jel burn dressings, and a moldable SAM splint for stabilizing fractures.